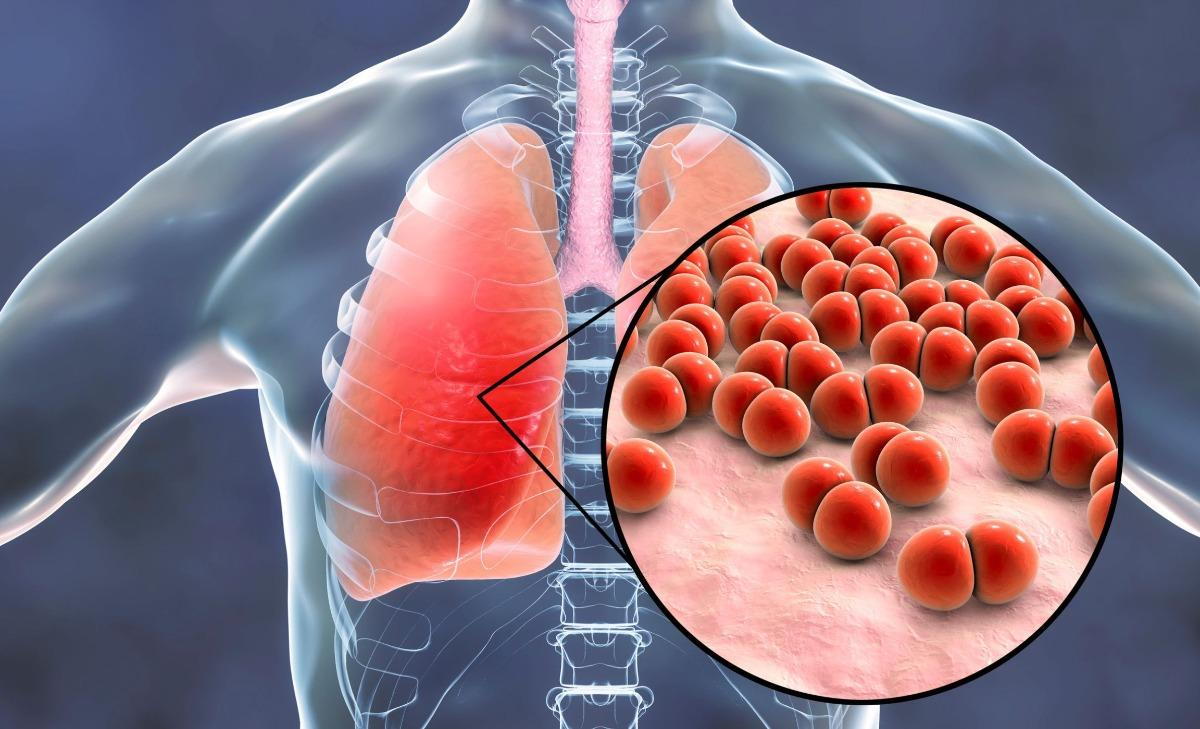
Pediatric pneumonia is a serious lung infection that affects children worldwide. The lungs, made up of tiny air sacs called alveoli, are responsible for oxygen exchange when you breathe. However, when a child has pneumonia, these alveoli fill with fluid and pus, making breathing painful and restricting oxygen intake. This condition is not only common but also the leading cause of death from infectious diseases in children. In fact, in 2019, pediatric pneumonia led to the death of over 740,000 children under five years old, accounting for a significant percentage of child mortality.
While pediatric pneumonia can be found globally, it is particularly deadly in regions like Southern Asia and sub-Saharan Africa. Despite its severity, pneumonia is preventable with simple interventions and can be treated effectively with accessible, low-cost medications. The causes of this kind of pneumonia vary, with bacteria, viruses, and fungi being the most common culprits.
Streptococcus pneumoniae and Haemophilus influenzae type B are the primary bacterial causes, while respiratory syncytial virus is the most prevalent viral trigger. In infants, particularly those with HIV, Pneumocystis jiroveci is a leading cause.
Pneumonia is spread through airborne droplets from sneezes or coughs and can also be transmitted through the blood, especially around birth. Understanding how pneumonia spreads and its various causes is critical to reducing its impact and providing the right care for children. By being aware of the symptoms and taking preventive measures with the help of McKinney pediatrics McKinney, TX experts, you can help protect your child from this serious and potentially life-threatening condition.
Common Symptoms of Pediatric Pneumonia

The signs and symptoms of pediatric pneumonia can range from mild to severe, and they often depend on factors like the type of germ causing the infection, as well as your child's age and overall health. In the early stages, pneumonia may present symptoms similar to those of a cold or flu, but unlike these viral infections, pneumonia tends to last longer and may worsen over time. If you notice any concerning signs in your child, it's important to consult with a McKinney doctor who can help determine the cause and recommend the appropriate treatment.
Common signs to watch for include chest pain when your child breathes or coughs, a persistent cough that might bring up phlegm, and fatigue. Fever, sweating, and chills are also typical symptoms, along with shortness of breath. In some cases, particularly in children under the age of two, pneumonia may not show clear symptoms at first. Instead, your baby may be more irritable, have trouble feeding, or show signs of restlessness and low energy. Newborns and infants are often unable to communicate their discomfort, so it’s crucial to keep a close eye on their breathing and behavior.
If your child has a persistent cough, difficulty breathing, or a fever that doesn’t subside, it’s important to seek medical attention. If your child’s fever reaches 102°F or higher, or if they start to exhibit chest pain or unusual lethargy, you should contact a healthcare provider immediately.
The best McKinney pediatrician can evaluate the symptoms and provide guidance on treatment, especially for children who may be at higher risk, such as those with underlying health conditions or weakened immune systems. It’s essential to take prompt action, as pneumonia can escalate quickly, and early intervention can prevent serious complications. Keep in mind that if your child is coughing up pus or showing signs of distress, it's time to see a McKinney doctor.
Risk Factors for Pediatric Pneumonia

Certain age groups are more vulnerable to pneumonia, making it essential to be aware of these risk factors. For adults, those aged 65 and older are at a significantly higher risk. As age increases, so does the likelihood of developing pneumonia. For example, an 80-year-old is at a much greater risk than someone who is 65.
For children, those younger than five years old are also at increased risk. A one-year-old child faces a higher risk than a four-year-old due to their developing immune systems and smaller airways. It’s important to keep in mind that both age groups are particularly susceptible and require extra care and attention. If you have concerns about your child's health, visiting a McKinney clinic can provide the guidance and care needed to address potential risks like pneumonia.
In addition to age, various chronic medical conditions can increase the risk of pneumonia. If someone has chronic heart disease, chronic liver disease, chronic lung disease, or diabetes, they are more likely to develop pneumonia.
These conditions make the body less able to fight off infections and can lead to complications. Individuals with weakened immune systems are also at heightened risk. Conditions such as HIV/AIDS, cancer, or medications like chemotherapy can suppress the immune system, leaving the body more vulnerable to respiratory infections. If your child has any of these conditions, it's important to seek advice from McKinney pediatricians who can provide specialized care and ensure your child stays protected from infections like pediatric pneumonia.
Certain behaviors can increase the chances of getting pneumonia as well. For instance, being around people who are sick, drinking alcohol excessively, or smoking cigarettes can all contribute to the risk. Fall and winter are typically when respiratory diseases, including pneumonia, spread most rapidly. However, pneumonia can occur at any time of the year, so it’s important to take preventive measures year-round. If you notice any symptoms in yourself or your child, consulting a McKinney doctor for guidance is crucial in preventing further complications.
How Pediatric Pneumonia is Diagnosed

To diagnose pneumonia, your healthcare provider will begin by asking about your medical history and performing a physical exam. They will listen to your lungs with a stethoscope to detect any abnormal sounds, such as crackling or wheezing, which could indicate pneumonia. Depending on your symptoms and exam results, your provider may recommend additional tests to confirm the diagnosis and determine the cause of the infection. One of the most common tests is imaging, such as a chest X-ray or CT scan, which helps your provider visualize the lungs and spot any signs of infection, like fluid buildup or consolidation. These images provide valuable insight into how much damage the pneumonia has caused.
A McKinney clinic may also perform pulse oximetry, a simple test that measures the amount of oxygen in your blood using a sensor clipped to your finger. This test helps determine how well your lungs are functioning and if your body is receiving enough oxygen. Blood tests are another important tool to help identify the infection and assess the severity of the condition. In some cases, a sputum test, where you’re asked to cough and spit into a container, may be used. The lab analyzes the sample to determine the bacteria or virus causing the infection.
If these tests don’t provide a clear answer, your provider may order more advanced tests, like a pleural fluid culture, where a sample of fluid around your lungs is taken for analysis, or an arterial blood gas test, which measures oxygen and carbon dioxide levels in your blood. In rare cases, a bronchoscopy might be needed to examine your lungs directly using a thin tube with a camera. All these tests work together to give your provider a comprehensive understanding of your condition and help them plan the best treatment for you.
Treatment and Recovery for Pediatric Pneumonia
When your child has viral pneumonia, the treatment typically focuses on rest and managing symptoms like fever. There is no specific medication for viral pneumonia, so your McKinney pediatrician will likely recommend fever control measures such as over-the-counter medications. It's important to avoid using cough suppressants like codeine or dextromethorphan, as coughing plays a crucial role in clearing the mucus and secretions that build up in the lungs during an infection. Though the cough may linger for several weeks, the rest of the symptoms usually improve after a few days.
Because it can be challenging to distinguish between viral and bacterial pneumonia based solely on symptoms, your pediatrician may prescribe antibiotics, especially if they suspect a bacterial infection. If antibiotics are prescribed, ensure your child completes the entire course as directed, even if they start feeling better quickly.
Discontinuing the medication prematurely can cause the infection to return. Additionally, there is a vaccine available to protect your child from pneumococcal infections, a common bacterial cause of pneumonia. The American Academy of Pediatrics recommends that children begin receiving the pneumococcal conjugate vaccine at 2 months of age, with doses administered at 2, 4, 6, and 12 to 15 months.
If your child missed any of the recommended doses, consult your pediatrician about a catch-up vaccination schedule. For children who have not received the pneumococcal vaccine by age 2, one dose is advised for healthy children aged 2 to 5 years, as well as for children with certain medical conditions. A second type of pneumococcal vaccine, the pneumococcal polysaccharide vaccine, is recommended for older children with high-risk factors, including those with heart or lung conditions, sickle cell anemia, or weakened immune systems, to help prevent pediatric pneumonia.

