
Roseola, also known as exanthem subitum or sixth disease, is a common viral infection that primarily affects infants and young children. It is characterized by a sudden high fever that lasts for a few days, followed by the appearance of a distinctive rash. The condition is typically caused by human herpesvirus 6 (HHV-6) and, less frequently, by human herpesvirus 7 (HHV-7). While roseola is generally mild and self-limiting, its abrupt onset and high fever can be concerning for parents.
The history of roseola dates back to the early 20th century when John Zahorsky Jr., a pediatrician, first described the illness in 1909. He presented his findings to the St. Louis Pediatric Society, detailing cases of fever accompanied by a rash in young children. In 1913, Zahorsky expanded on his research in an article for the Journal of the American Medical Association (JAMA), highlighting the need to differentiate roseola from other febrile illnesses, particularly rubella.
Over time, additional studies confirmed that roseola was a distinct condition. In 1921, Veeder and Hempelmann established it as a separate disease entity, introducing the term “exanthem subitum.” Later, in 1936, Swiss pediatrician Jules-René Dreyfus referred to it as "sixth disease," a name that persists today.
Despite its long history, the specific viral cause of roseola remained unknown until 1988, when Yamanishi et al. successfully isolated HHV-6 from the blood of infected patients. This breakthrough allowed pediatricians to confirm that the virus was the primary cause of the illness.
Since then, medical understanding of roseola has continued to evolve, helping pediatricians diagnose and manage the condition more effectively. In the following sections, we will explore the symptoms, transmission, diagnosis, and treatment of roseola in greater detail.
Causes and How It Spreads

While these viruses belong to the herpes family, they do not lead to conditions like cold sores or genital herpes. Instead, they specifically target young children, causing a temporary illness marked by fever and rash.
Who Is Most at Risk?

Roseola primarily affects infants and toddlers, with the highest incidence occurring between 6 and 15 months of age. Most cases occur in children under the age of 3, as older children and adults typically develop immunity.
How Roseola Spreads

The virus spreads easily through respiratory droplets released when an infected person talks, laughs, sneezes, or coughs. Direct contact, such as sharing drinks or utensils, can also facilitate transmission. Additionally, the virus can survive on surfaces, meaning that touching contaminated objects and then touching the face can lead to infection. If your child shows concerning symptoms, a visit to a pediatric urgent care center can help with prompt evaluation and management.
Contagious and Incubation Period

Children with roseola are most contagious during the fever stage, even before the rash develops. Once exposed, symptoms may take anywhere from 5 to 15 days to appear.
Although roseola is generally mild, it can occasionally cause febrile seizures due to the sudden rise in body temperature. Fortunately, these seizures are usually brief and do not cause long-term harm.
There is no specific antiviral treatment for roseola, so management focuses on symptom relief, such as reducing fever and keeping the child hydrated. A pediatrician can provide guidance on supportive care to ensure a smooth recovery. After the fever subsides, a distinctive rash may develop on the chest, back, and belly before spreading to the neck and trunk. Once a child has recovered, they typically develop lifelong immunity, preventing future infections.
Roseola: The Two Stages
Stage 1: High Fever

Roseola typically starts with a sudden spike in temperature, often reaching 103°F (39.4°C) or higher. This fever can persist for three to five days before resolving. During this phase, children may also experience mild respiratory symptoms such as a runny nose or cough, as well as gastrointestinal issues like diarrhea or vomiting.
Some children become irritable or fussy due to the fever. This is the most contagious stage of the illness, as the virus is actively spreading through respiratory droplets and close contact. If symptoms become severe or concerning, visiting a pediatric clinic can help ensure proper evaluation and care.
Stage 2: Rash Development
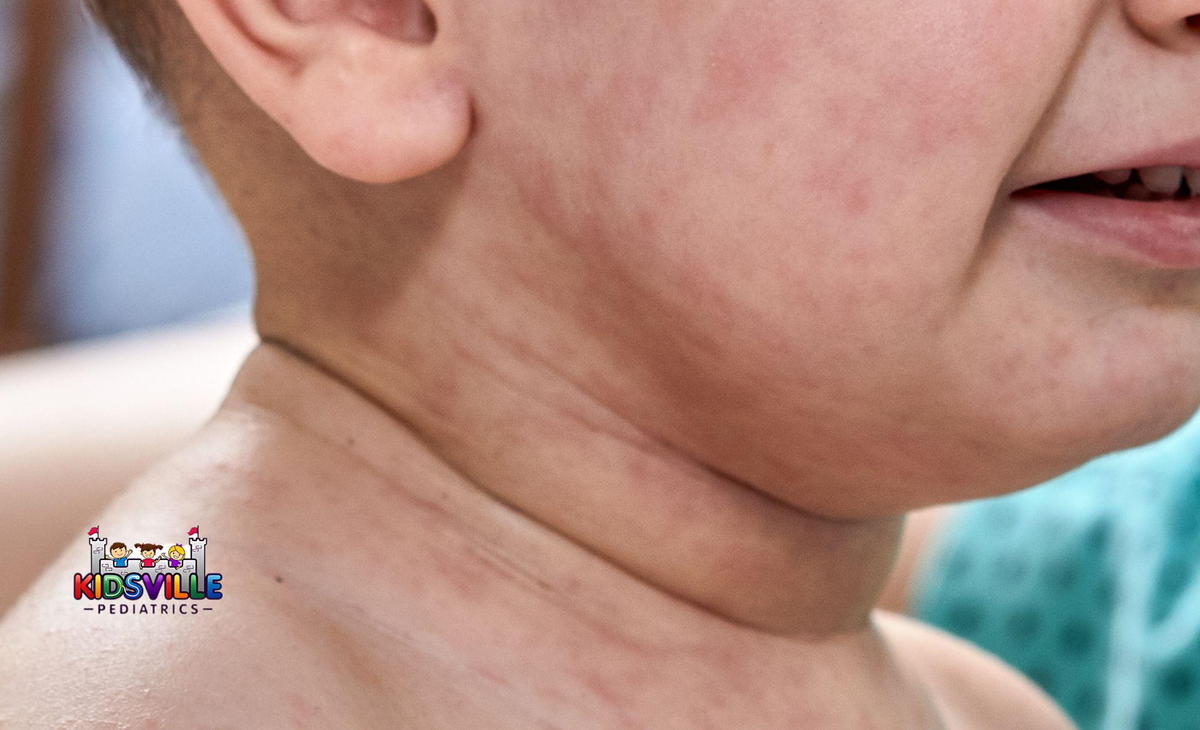
As the fever subsides, a pink or reddish rash begins to emerge. The rash consists of small, flat, or slightly raised spots, which may appear in clusters. It typically starts on the chest and back before spreading to the neck, arms, face, and legs.
Unlike the fever phase, children are no longer considered contagious once the rash appears. The rash itself is painless and does not cause itching or discomfort. It can last anywhere from a few hours to a couple of days before gradually fading away. If you have concerns about your child’s symptoms, a pediatric center can provide expert evaluation and guidance.
Recovery and Outlook
Most children recover completely within a week, with no lasting effects. Once a child has had roseola, they usually develop immunity and are unlikely to get it again. While the illness can be unsettling due to the high fever, it is generally mild and resolves on its own with supportive care.
When to See a Pediatrician
While roseola is generally mild, certain symptoms warrant pediatric urgent care. If your child experiences a febrile seizure—a seizure triggered by high fever—seek emergency care right away. Additionally, contact a pediatrician if your child's symptoms worsen or fail to improve within a week.
Other signs that require medical evaluation include:
High Fever: If your child’s fever exceeds 103°F (39.4°C), it’s important to consult a healthcare provider.
Recurrent Fever: If the fever returns after the rash has disappeared, seek medical advice.
Persistent or Worsening Rash: If the rash worsens or doesn’t start fading within 4-5 days, or if it persists for several weeks, a doctor should assess the condition.
Lethargy or Unresponsiveness: If your child becomes excessively sleepy, difficult to wake, or unusually unresponsive, medical attention is necessary.
Dehydration Signs: If your child has reduced urine output, refuses to drink, or won’t breastfeed, they may be dehydrated and need medical support.
Unusual Weakness or Fatigue: If your child appears weaker or less active than usual, it may indicate a complication that requires medical assessment.
Weakened Immune System Exposure: If anyone in the household has a weakened immune system and comes into contact with someone with roseola, they should be monitored for signs of infection, as their illness could be more severe.
Doctors typically diagnose roseola based on symptoms and medical history rather than extensive testing. The illness presents with a sudden high fever, often reaching 104°F (40°C), which lasts 3-5 days. As the fever resolves, a pink, non-itchy rash appears, usually beginning on the trunk before spreading to the arms and legs.
During a physical exam, a pediatrician will assess these hallmark symptoms and may ask about recent illnesses or exposure to infected individuals. In cases where symptoms are unclear or a definitive diagnosis is needed, a blood test may be conducted to confirm the presence of human herpesvirus 6 (HHV-6) or HHV-7, the viruses responsible for roseola.
By staying vigilant and knowing when to seek medical attention, parents can help ensure a smooth recovery from roseola for their child.

