Jaundice in newborns is a common condition that often causes alarm in parents, especially first-timers. It usually develops during the first week after birth and shows up as a yellow tint on the baby’s skin and the whites of their eyes. This yellowing occurs due to an excess of bilirubin, a yellow pigment produced during the normal breakdown of red blood cells. While it is usually harmless and resolves on its own, understanding its causes, types, treatments, and when to worry is important for every caregiver.
What Causes Newborn Jaundice?

Jaundice in newborns occurs because babies have more red blood cells than adults, and these cells break down and get replaced more often. Because their liver is still developing, it may not yet be able to clear bilirubin from the bloodstream effectively. This causes bilirubin to accumulate in the body, resulting in the noticeable yellow coloring of the skin and eyes.
There are several types of jaundice, each with different causes:
Physiological jaundice is the most common type, occurring in more than half of all newborns. It generally appears on the second or third day of life and resolves without treatment within two weeks.
Breastfeeding jaundice can occur in breastfed infants during the first week if the baby isn’t getting enough breast milk. It’s not caused by breast milk itself but by inadequate feeding.
Breast milk jaundice typically appears in the second week and may last for several weeks or even longer. It's believed to be linked to substances in the mother's milk that slow the processing of bilirubin.
Hemolytic jaundice results from blood group incompatibility between the mother and baby, such as Rh or ABO incompatibility, leading to increased red blood cell breakdown.
Pathologic jaundice appears within the first 24 hours after birth or involves very high bilirubin levels. This type requires urgent medical evaluation by a qualified pediatrician in Mansfield TX.
Symptoms and Diagnosis

The primary sign of jaundice is yellowing of the skin and eyes. It generally begins on the face and then spreads down to the chest, belly, and legs. Parents can try gently pressing the baby's skin — if it appears yellow where pressed, it may indicate jaundice.
Doctors diagnose jaundice by:
Visual examination
Bilirubin blood test (called serum bilirubin level)
Transcutaneous bilirubinometer (a device placed on the skin to estimate bilirubin levels)
n severe or unusual cases, a doctor in Mansfield may order additional tests to identify the underlying cause or assess for complications.
Risk Factors

Certain factors increase the likelihood of a newborn developing jaundice:
Premature birth (before 37 weeks gestation)
Bruising during birth or a traumatic delivery
Blood type incompatibility between mother and baby
A sibling who had jaundice
Ethnic background (East Asian babies are more prone)
Inadequate breastfeeding
It’s important for parents to recognize these risk factors early so they can monitor their baby closely and consult a Mansfield pediatrician if necessary.
Treatment Options

Treatment depends on the bilirubin level, the baby’s age in hours, and whether the baby was born early. For mild cases of jaundice in newborns, treatment might not be necessary. The condition can resolve naturally as the baby’s liver matures and the baby starts feeding regularly, which helps flush out bilirubin.
However, if bilirubin levels are high or continue to rise, medical intervention may be required:
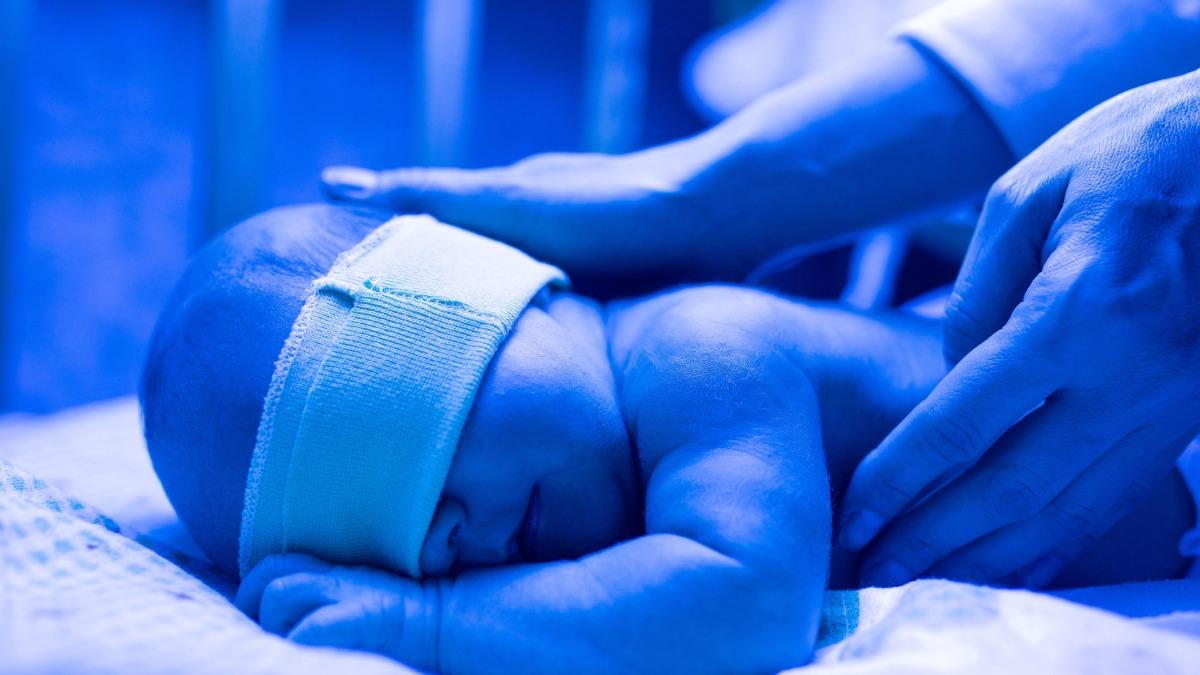
Phototherapy: The baby is placed under a special light that helps break down bilirubin in the skin. It’s the most common treatment and is usually very effective.
Exchange transfusion: In severe cases, the baby’s blood may be replaced with fresh donor blood to quickly lower bilirubin levels.
IV fluids: Sometimes used to aid hydration and support the body’s ability to process bilirubin.
Parents are often encouraged to feed the baby frequently (8-12 times a day) to promote bilirubin elimination through the digestive system.
When to Worry
While most cases are harmless, untreated severe jaundice can lead to a rare but serious condition called kernicterus. This occurs when excessive bilirubin enters the brain, potentially causing permanent brain damage. Symptoms of severe jaundice include:
High-pitched crying
Poor feeding or difficulty waking
Limpness or extreme stiffness
Any of these signs warrant immediate medical attention.
Prevention and Monitoring
While jaundice in newborns cannot always be prevented, certain measures can help reduce its severity or the likelihood of complications:
Ensure effective breastfeeding from the first few hours of life.
Schedule early checkups — most pediatrician Mansfield experts recommend a newborn be seen within 3 to 5 days after birth.
Monitor for yellowing skin and eyes daily in the first week.
Hospitals now routinely screen for jaundice before babies are discharged. Still, some cases don’t appear until the baby is at home, so awareness remains crucial.
Supporting Parents Through Newborn Jaundice

A jaundice diagnosis can be worrying for many families. However, with guidance from pediatricians, most babies recover quickly and without lasting effects. It helps to educate caregivers in advance so they know what signs to watch for and feel confident about treatment decisions. Nurses, pediatricians, and lactation consultants often provide invaluable support during this phase.
In conclusion, while jaundice in newborns can be worrisome at first, it is usually a manageable and short-term condition. Understanding the symptoms, risk factors, and treatments empowers parents to respond confidently and effectively. As always, regular follow-ups with a pediatrician are key to ensuring a healthy start to your baby’s life.

