
At Kidsville Pediatrics, families often ask about the APGAR score that doctors mention right after a baby is born. This quick assessment tool plays an essential role in evaluating a newborn’s immediate health status, offering a structured way to check how well the baby is transitioning to life outside the womb.
Parents who visit our McKinney clinic can rest assured that our team of highly trained pediatricians uses evidence-based practices—including tools like the APGAR score—to ensure infants receive the safest start possible.
History and Development of the APGAR Score
 Public Domain: Dr. Virginia Apgar
Public Domain: Dr. Virginia Apgar
The APGAR score came into existence in 1952 through Dr. Virginia Apgar who was an American anesthesiologist who saw the need for a standard in the assessment of newborns right after birth. Before her innovation, doctors and nurses lacked a consistent way to measure a newborn’s physical condition right after birth.
Dr. Apgar developed a simple, five-component scoring system that could be performed quickly and repeatedly. Over the decades, the tool has undergone refinement and widespread adoption, becoming one of the most recognized and utilized assessments in neonatal medicine. Even now, it remains a cornerstone of newborn evaluation, though modern medicine has expanded beyond it with additional diagnostic methods.
Components of the APGAR Score

The acronym APGAR corresponds to five key indicators of a newborn’s health:
Appearance (skin color): Checks whether the baby’s skin tone is pale, bluish, or pink, indicating oxygenation and circulation.
Pulse (heart rate): A rapid pulse over 100 beats per minute reflects strong cardiovascular function.
Grimace (reflex irritability): Evaluates the baby’s response to stimulation, such as a gentle pinch or suction.
Activity (muscle tone): Observes whether the baby is limp, shows some flexion, or moves actively.
Respiration (breathing effort): Determines whether the baby is not breathing, breathing weakly, or crying vigorously.
Each of these five elements is scored on a scale from 0 to 2, with higher scores indicating better adaptation. Together, these categories provide a snapshot of the baby’s overall condition.
Scoring Methodology and Interpretation
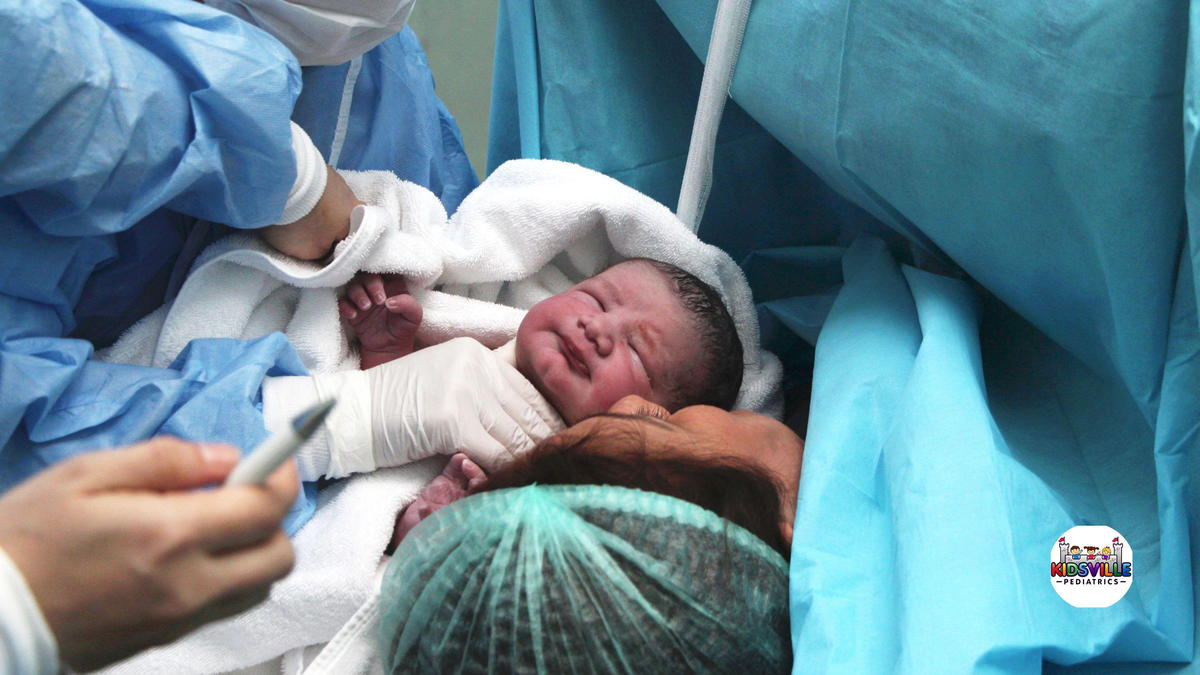
The APGAR score is assessed at one minute and again at five minutes after birth. In some cases, additional scores may be recorded at 10 minutes. The total score ranges from 0 to 10.
7–10: Generally reassuring, showing the newborn is adapting well.
4–6: Indicates moderate difficulty; the infant may need assistance such as oxygen or stimulation.
0–3: Suggests severe distress, requiring immediate resuscitative efforts.
It is important for parents to understand that a low one-minute score does not necessarily predict long-term health problems. Many babies improve significantly by the five-minute assessment.
Clinical Applications and Limitations
The APGAR score remains invaluable for guiding immediate medical interventions. It provides healthcare providers—including any pediatrician McKinney expert families may see at our practice—with a structured way to decide whether a newborn needs help with breathing, circulation, or other vital functions.
However, the score does have limitations. It was never designed to predict long-term developmental outcomes or neurological health. Misinterpretation sometimes leads parents to worry unnecessarily if their baby’s early score is low. In reality, the APGAR score is meant to guide urgent clinical care in the delivery room, not to serve as a forecast of the child’s future abilities.
Alternatives and Modifications to APGAR
While the APGAR score remains widely used, medicine has advanced with alternative and supplemental assessments. For example, preterm infants may not score as highly simply due to immaturity, so modified scoring systems have been proposed. In addition, tools such as the Neonatal Resuscitation Program (NRP) guidelines provide structured interventions beyond what APGAR alone can guide. These newer methods enhance neonatal care while still respecting the foundation laid by Dr. Virginia Apgar’s original system.
Choosing Quality Pediatric Care in McKinney
At Kidsville Pediatrics, we believe that education helps parents feel confident in their child’s care. Whether discussing the APGAR score, growth milestones, or vaccinations, our team works closely with families to provide clarity and reassurance.
If you are searching for the best pediatrician in McKinney TX, look no further than our compassionate providers, who blend clinical expertise with personalized care.
From your baby’s very first breath, our McKinney doctor team is here to monitor, support, and nurture your child’s health. The APGAR score is just one of many tools we use to make sure newborns begin life with the best possible care. With experienced McKinney pediatricians by your side, you can trust that your family is in safe, skilled hands.

